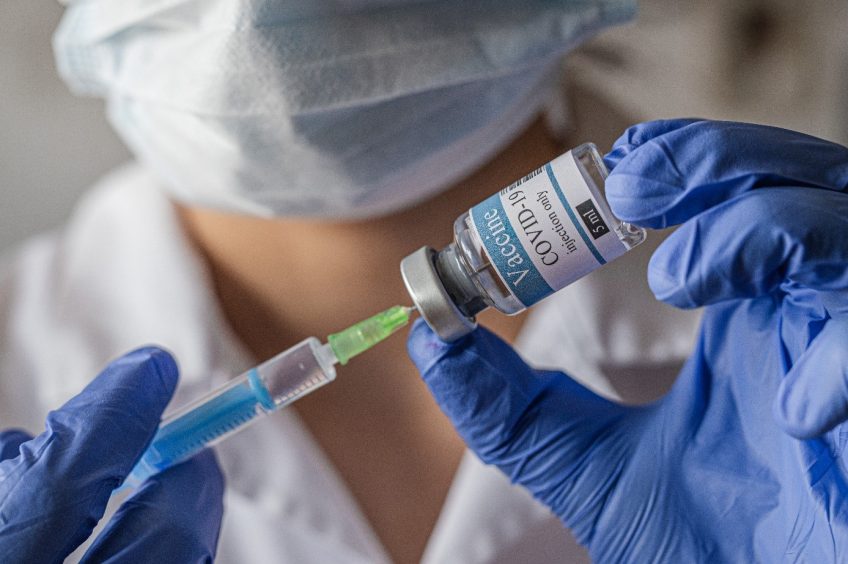
Researchers have found that the COVID-19 mRNA vaccines that saved millions of lives during the pandemic may also help the immune system fight cancer. Scientists from the University of Texas MD Anderson Cancer Center and the University of Florida say that patients with advanced cancer who received either the Pfizer or Moderna COVID-19 vaccine showed much better survival rates when undergoing immunotherapy.
The study, published in Nature and presented at the 2025 European Society for Medical Oncology (ESMO) Congress in Berlin.
Researchers examined data from more than 1,000 cancer patients treated at MD Anderson between 2019 and 2023. These patients had late-stage melanoma or lung cancer and were receiving a type of treatment known as immune checkpoint inhibitors. These drugs help the immune system recognize and attack cancer cells more effectively.
The team discovered that patients who got the mRNA COVID-19 vaccine within 100 days of starting immunotherapy were twice as likely to be alive three years later compared to those who never received the vaccine. The average survival for vaccinated patients was 37.3 months, while it was only 20.6 months for those who did not get vaccinated.
Patients with “cold” tumor cancers that usually do not respond well to immunotherapy also showed major improvements. Their survival rates increased nearly five times compared to similar patients who did not get the vaccine. This shows that the vaccine helped the immune system recognize and attack tumors that were previously ignored.

Dr. Elias Sayour, a pediatric oncologist at the University of Florida who led part of the study, explained “mRNA vaccines that are not specific to a patient’s cancer can wake up the sleeping giant that is the immune system,” he said. “When that happens, the body starts recognizing and killing tumor cells that it used to ignore.”
The study team also ran experiments on animals to understand how this works. They found that the mRNA vaccine acts like an alarm for the immune system. It makes the body alert and ready to fight. When this happens alongside immunotherapy drugs, the immune system becomes much more powerful and can attack cancer cells more aggressively.
“When a patient receives an mRNA vaccine, it doesn’t just prepare the body to fight a virus, it also trains the body to detect other threats like cancer cells,” said Dr. Sayour.
Dr. Adam Grippin, a physician-scientist at MD Anderson and one of the lead authors of the study said, “This study shows that commercially available mRNA COVID vaccines can train patients’ immune systems to eliminate cancer,” he said. “When combined with immune checkpoint inhibitors, these vaccines produce strong antitumor responses and major improvements in survival for cancer patients.”
Immunotherapy has changed the way doctors treat many cancers, but it does not work for everyone. By adding an mRNA vaccine, scientists believe many more patients could benefit. Fox News medical analyst Dr. Marc Siegel said, “This shows the potential for mRNA vaccines to work together with immunotherapy to target certain proteins in cancer and possibly improve survival. These vaccines could become an important tool in a more personalized approach to cancer.”
The researchers are now preparing a nationwide clinical trial through the UF-led OneFlorida+ Clinical Research Network. This trial will include hospitals and clinics across Florida, Alabama, Georgia, Arkansas, California, and Minnesota.
Patients with lung cancer will be randomly divided into two groups — one will receive a COVID-19 mRNA vaccine during immunotherapy treatment, and the other will not. The goal is to see if the vaccine should become part of standard cancer care.
“If a widely available and low-cost vaccine can improve cancer survival, it could revolutionize cancer therapy,” Dr. Sayour said. “Even a 10 percent improvement in survival would mean thousands of lives saved. Imagine if we could double that.”
The researchers also point out that, unlike custom-made cancer vaccines, which are expensive and take months to produce, COVID-19 mRNA vaccines are already widely available. They can be given quickly, easily, and affordably anywhere in the world. This makes them a realistic option even in countries with limited medical resources.
Dr. Steven Lin, co-author of the study and professor of Radiation Oncology at MD Anderson, said, “This discovery shows how a tool created during the pandemic can be used to fight another deadly disease. What started as a weapon against a virus could now help us battle cancer.”
The study was supported by several organizations, including the National Institutes of Health, the National Cancer Institute, the Food and Drug Administration, and the American Brain Tumor Association. It represents a new hope for millions of patients worldwide. The simple COVID-19 vaccine that once protected humanity from a pandemic might soon help it overcome one of its oldest and deadliest cancers.